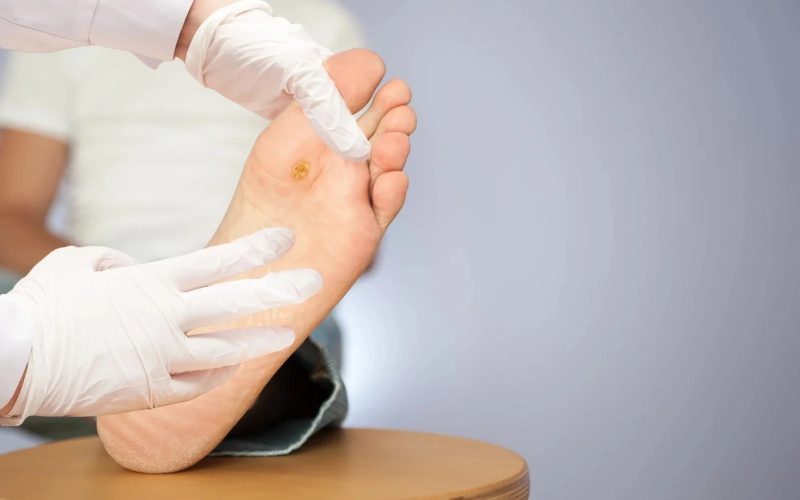
The frustration of a persistent foot lesion can be attributed to a series of temporary relief and the immediate return of the problem. From a localised pressure point to a viral cluster, many individuals have found that the over-the-counter treatments often hit a brick wall.
This is because the skin on the soles of the feet is unique. It is the thickest part of the human body and is constantly subjected to gravitational pressure. When a lesion fails to respond to initial care, it is typically classified as recalcitrant.
Understanding why this happens requires looking beneath the surface at the biological and mechanical factors that shield these conditions from basic pharmacy-bought solutions. Seeking professional corn or verruca removal in London is often the only way to bypass these defensive barriers and reach the living tissue where the pathology resides.
So, take a look at the seven reasons your foot lesion has become treatment-resistant.
1. The Basement Membrane Barrier
The primary reason most topical paints and gels fail is a matter of depth.
The skin is composed of multiple layers, and both the HPV virus (which causes verrucas) and the keratinised plug of a corn sit deep within the dermis or at the basement membrane. Standard salicylic acid treatments are designed to peel the top layer of dead skin.
However, if the treatment cannot penetrate the full thickness of the stratum corneum, the factory at the base remains untouched. In these cases, the top layer is removed, but the root remains, allowing the lesion to regenerate almost as quickly as it is treated.
2. The Protective Hyperkeratotic Shield
The body recognises the presence of a chronic lesion as if it were a foreign body or a site of injury. In response, the body makes extra keratin to provide protection. It forms a thick, hard callus, like a suit of armor.
In the case of the verruca, the armor prevents the medicine from penetrating. In the case of the corn, the extra skin actually makes the pressure greater, driving the lesion deeper into the foot.
Without the process of debriding, or shaving off the extra skin, the medicine simply remains on the surface, unable to reach the active site of the infection or the pressure point.
3. The Immune-Privileged Nature of the Virus
Verrucas are particularly insidious because they are low-grade infections. In other words, unlike with flu or a bacterial infection in a wound, the HPV virus does not enter the blood system. Instead, it remains in the skin cells, or keratinocytes, hiding from the white blood cells, which are part of the immune system.
The immune system completely ignores this infection because it has no idea it is there, which is why it can remain for so long without being fought off by the body. The medical treatments, such as needling or using a high-powered laser, are intended to create a micro-injury, which will, in turn, alert the immune system to the presence of the virus.
4. Nucleated Density and Nerve Entrapment
When a corn changes from a simple callus to a hard corn, a nucleus will form. The nucleus is a dense, cone-shaped plug of keratin. In time, this dense nucleus will start to push the surrounding tissue out of the way, and in some cases, this will include nerve endings or small vessels. This type of corn is called a neurovascular corn. At this point, the corn is no longer purely a skin problem, but a neurological one. The acids found in most corn plasters will do nothing but harm the surrounding tissue, leaving the nerve-pressing nucleus completely untouched.
5. Biomechanical Feed Loops
The most overlooked reason for treatment resistance is the way a person walks.
A corn is essentially a symptom of mechanical friction. If a patient has a hammer toe, a dropped metatarsal, or an unstable gait, that specific area of the foot will always be under attack. Even the most successful corn removal treatment in London will only provide temporary relief if the mechanical cause isn’t addressed.
The skin is simply doing its job by thickening in response to pressure; until that pressure is diverted through better footwear or orthotics, the lesion will continue to reform as a biological defense mechanism.
6. The Koebner Phenomenon in DIY Care
Most people unknowingly make lesions more difficult to treat when attempting “bathroom surgery.” When a person tries to excise a verruca with unsterilized tools, they create trauma to the surrounding skin, increasing the risk of the Koebner phenomenon.
The Koebner phenomenon refers to the development of new lesions in areas of skin injury. Rather than eliminating the virus, this trauma can lead to its spread into adjacent tissue (autoinoculation), resulting in multiple clustered lesions, often referred to as mosaic verrucae.
This increased viral burden makes subsequent professional treatment more challenging, as the infection is no longer localized but distributed across a wider surface area.
7. Chronic Vascularisation
As the lesion becomes a chronic condition, the body may respond by producing new small blood vessels that supply the overactive skin growth. This is often the case in a chronic verruca, as indicated by the small black dots that are thrombosed vessels, which are visible after the surface is pared back.
The new vessels supply the lesion with a constant source of food, making the lesion resistant to cold treatments like cryotherapy after the surface is debrided back.
At this stage, the lesion is well established and requires precise clinical treatment to cauterise the feeding capillaries and disrupt the underlying tissue sustaining the lesion.
Final Thoughts
Breaking the cycle of a treatment-resistant foot lesion requires moving beyond the peel-and-hope method. By understanding the histological depth and the mechanical triggers involved, it becomes clear that persistent corns and verrucas are not just stubborn skin; they are complex biological structures that require a targeted, multi-layered clinical approach to resolve permanently.
So, keep these in mind to avoid inadvertently making your verrucas or corn treatment-resistant.